What Causes Gingivitis and How to Stop It?
What is Gingivitis?
Gingivitis refers to inflammation and bleeding of the gums, and can be an early form of periodontal disease, definitely a scary-sounding term. While “Gingivitis” sounds like an exotic new concoction from a swanky cocktail bar, it actually refers to something more sinister, and slightly scary. Periodontal disease, destroys the tissues that support the teeth — the gums, the periodontal ligaments, and the tooth sockets, and can lead to bone loss, which is irreversible. The nasty endpoint of all this? Our teeth can fall out, just like that.
But how do we get from bleeding gums to no teeth? If we don’t treat gingivitis early, the area can become so infected that the gum attachment and bone around the tooth is destroyed. It sounds icky, but food can then get trapped under the gums and tartar builds up at the base of the tooth. The tooth finally becomes loose and it’s denture time for us!
So, it is crucial to treat gingivitis before it causes periodontal problems.
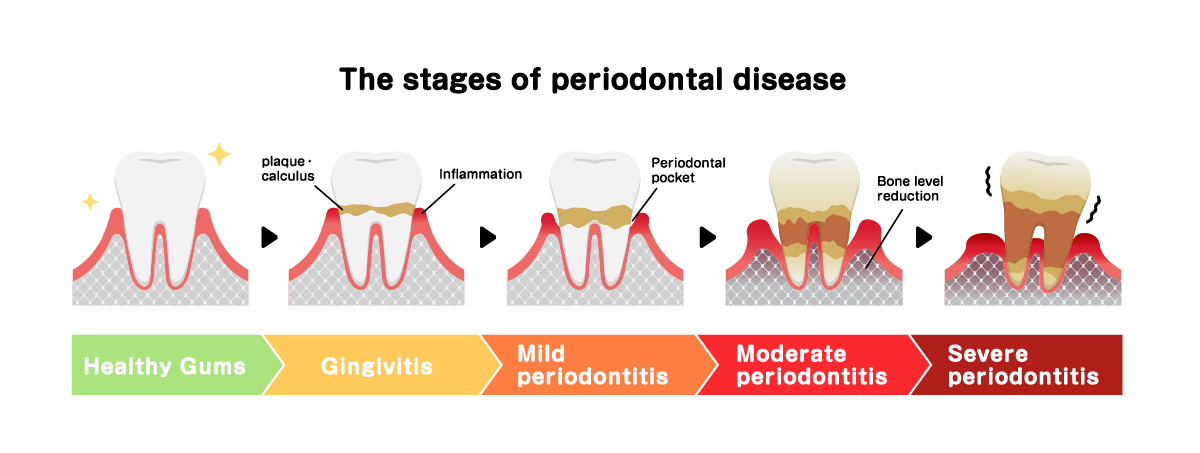
How common is gingivitis?
According to the US’ National Health and Nutrition Examination Survey (NHANES),
47 per cent of adults have gum disease. In adults 65 and older, this increases to 70 per cent.* As with many other annoying ailments, gingivitis becomes more of an issue with age, but we all need to be kind to our teeth and watch out for the signs of gingivitis.
The tricky thing about gingivitis is it’s rarely painful in its early stages, so it often goes unnoticed until there is severe irritation or receding gums. Many people have gingivitis to some degree.
How do I know if I have gingivitis?
If gingivitis is so common and can be so invisible, what are the signs that it’s creeping up on your teeth and gums? Some telltale signs are:
- – swollen gums
- – soft, puffy gums
- – receding gums
- – tender gums
- – gums that bleed easily when you brush or floss (you can see this as redness or pinkness on your toothbrush or floss)
- – a change in gum colour from a healthy pink to dusky red
- – bad breath
Where does gingivitis come from?
The choice of toothpaste will determine the condition of your mouth. It is important to choose the best toothpaste for gingivitis because poor oral hygiene will create plaque deposit. Plaque is the sticky stuff that sits on our teeth. It’s a delightful combination of bacteria, mucus, and food debris that naturally develops on the teeth and it is a major cause of tooth decay. If we don’t remove plaque by brushing and flossing, within 72 hours it will harden into a deposit that becomes trapped at the base of the tooth. That’s what the dentist chips away at when you’re lying in the chair trying to open wiiiiiiide!
Plaque and tartar (P&T) irritate and inflame the gums. Bacteria and toxins produced from P&T cause the gums to become infected, swollen and tender. P&T is definitely not a new beverage from that cocktail bar!
What else causes gingivitis?
Apart from the build-up of plaque and tartar, gingivitis can occur whenever our gums are injured. We can even cause gingivitis ourselves being too eager when clean our teeth; overly vigorous brushing or flossing can damage sensitive gums and lead to bleeding and infection. We must treat our gums and teeth with TLC (now, that could be a new cocktail!)
Unfortunately, your risk of developing gingivitis increases if you have:
- – General illness
- – Hormonal changes, such as pregnancy or menopause, which increase the sensitivity of the gums
- – Uncontrolled diabetes
- – Misaligned teeth, rough edges of fillings, or ill-fitting or unclean mouth appliances
- – Braces, dentures, bridges and crowns
Medication such as phenytoin and birth control pills, and heavy metals such as lead and bismuth are also associated with gingivitis.
What happens if I don’t treat Gingivitis?
Since that scary periodontal disease (periodontitis) evolves from gingivitis, it is vital to tackle gingivitis symptoms before they cause irreversible problems.
We really don’t want periodontal disease because it can literally take the smile off our face by making our teeth fall out. Tooth loss makes everyday things like talking, chewing and swallowing more difficult. Tooth replacement options are often hard to adjust to and are just never as comfortable as your natural teeth. Remember, bone loss from gum disease is irreversible, so it is vital to treat gingivitis as soon as any symptoms appear.
More Gingivitis dangers – sorry!
Apart from being the cause of periodontal disease, gingivitis and gum disease have a clear link to heart disease. Those with gum disease have a 25 per cent greater risk of heart disease than those with healthy gums and 2004 study found that 91 per cent of patients with cardiovascular disease also had moderate to severe periodontal disease†.
This seems like a weird correlation but researchers have begun to uncover possible causes for the link. They now believe that gum disease, which is inflammatory, causes the release of pro-inflammatory chemicals into the bloodstream and this triggers an inflammatory response throughout the body.
The theory was further supported by a recent study of 5,000 participants, which showed that oral inflammatory markers entering the bloodstream also encouraged systemic inflammation♢. This large study also confirmed that when assessing the risk of heart disease, periodontal disease and body mass index are both associated with increased levels of CRP (C-reactive protein), which is made by the liver and increases when there inflammation somewhere in the body.
So it seems Gingivitis and gum disease are bad news for the whole body, and not just our gums and teeth.
How Do I Prevent Gingivitis?
Now that we’re scared into action, let’s get to the solution. And no, the solution is not a P&T cocktail to calm your nerves. Even if you already have some symptoms of gingivitis, don’t despair, just make sure you get started with the following steps:
- Choose Natural Toothpaste for Gingivitis
With so many toothpastes available in the market, it is not easy to find the best toothpaste for gingivitis. But Oral Botanica has been tested by Temasek Polytechnik that it has natural antibacterial that make it the best toothpaste for gingivitis. It is able to kill the unwanted bacterial while keeping the good bacteria in check.
- Proper Brushing
Brushing the gumline (at the base of the tooth) helps remove bacteria. Use a high quality, soft toothbrush with gentle bristles for your delicate gum tissue. Brush at least twice each day for two minutes each time.
- Flossing
No matter how well you brush, you’ll never be able to remove bacteria under the gums without flossing. Wrap the floss around the tooth and slide the floss up and down under the gumline. You can also use a floss pick or water flosser. Floss at least once a day to remove debris from under the gums and between the teeth, where a brush won’t reach - Healthy diet
A diet rich in key vitamins and fresh vegetables can improve your immune system and reduce infection in the body. DHA, vitamin C, iron and fibrous fruit all increase blood supply, boost the immunity and speed up healing. - Stop smoking
If you’re suffering from gum disease, smoking is one of the worst things you can do for your mouth. It is rare to see any type of healing take place in smokers’ mouths. The sooner you kick the habit the better for you and your oral health. - Regular Dental Checks
Regular visits to the dentist for cleaning will remove plaque and tartar build-up. If your mouth is healthy, visit the dentist for cleaning every 6 months. If you have active gum disease, you may need to have a dental check 3 to 4 months until the symptoms are reversed.
Use Oral Botanica Classic to prevent Gingivitis!

Oral Botanica Classic liquid toothpaste is a completely safe and effective oral care product. It is 100% organic, made with food-grade botanical oils. Oral Botanica is recognised by dentist as the best antibacterial toothpaste for gingivitis.
Daily use of the Oral Botanica Classic as a 3-in-1 toothpaste, mouthwash and breath freshener eliminates bacteria commonly associated with destructive gum disease.
The six potent botanical oils in Oral Botanical Classic can reach bacteria living in gum pockets, on the tongue and on the roof and walls of the mouth, place conventional toothpaste cannot reach.
Once you use Oral Botanica Classic regularly, plaque builds up more slowly than for those using conventional toothpaste.
Treating Gingivitis step by step

Step 1: Floss your teeth after every meal.
|

Step 2: Brush your teeth with 2 drops of |

Step 3: Dilute 3-5 drops Oral Botanica Classic with |
Good oral care habits and the right choice of toothpaste such as Oral Botanica Classic, you’ll be able to use your own healthy teeth and gums to take big bite out of life for many years to come.
*Eke, P.I., Dye, B.A., Wei L., Thornton-Evans, G.O., Genco, R.J. (2012) Prevalence of Periodontitis in Adults in the United States: 2009 and 2010. Journal of dental research.91:10. Retrieved from: https://journals.sagepub.com/doi/abs/10.1177/0022034512457373
† Geerts, S.O., Legrand, V., Charpentier, J., Albert, A., Rompen, E.H. (2004).Further evidence of the association between periodontal conditions and coronary artery disease. Journal of Periodontology, 75 (9), 1274-80. Retrieved from https://pubmed.ncbi.nlm.nih.gov/15515345/
♢ Noack, B., Genco, R.J., Trevisan, M., Grossi, S., Zambon, J.J., De Nardin, E. (2001). Periodontal Infections Contribute to Elevated Systemic C‐Reactive Protein Level, Journal of Periodontology, 72 (9), 1221-1227. Retrieved from https://aap.onlinelibrary.wiley.com/doi/10.1902/jop.2000.72.9.1221